
A few days ago, an Instagram post related to the death of model-actress Poonam Pandey created a buzz all around the country. News of her demise brought skepticism and grief to the fans, where her Instagram post stated:
“This morning is a tough one for us. Deeply saddened to inform you that we have lost our beloved Poonam to cervical cancer. Every living form that ever came in contact with her was met with pure love and kindness. In this time of grief, we would request for privacy while we remember her fondly for all that we shared.”
Poonam Pandey, began her career as a model in 2010 as a model. She became one of the top nine contestants of the Gladrags Manhunt and Megamodel Contest and appeared on the cover page of the fashion magazine. She is known for her contributions to the entertainment industry where she gained popularity through her appearance in various projects. You may remember her from the first season of Lock Upp hosted by Kangana Ranaut.
In 2020, for a brief time she was in limelight due to her unexpected marriage to Sam Bombay. She was a huge social media figure who appeared in few of the Bollywood films. Initially, she gained popularity because of her controversial posts. You may have come across her work in some of the Bollywood films like The Journey of Karma (2018) and Nasha (2013).
However, in a subsequent video statement, she revealed that the announcement was a stunt to create awareness about cervical cancer. Where she explained her purpose bind this act of her own demise. She said:
“I am here, alive. Cervical Cancer didn’t claim me, but tragically, it has claimed the lives of thousands of women who stemmed from a lack of knowledge on how to tackle this disease. Unlike some other cancers, Cervical Cancer is entirely preventable. The key lies in the HPV vaccine and early detection tests. We have the means to ensure no one loses their life to this disease. Let’s empower one another with critical awareness and ensure every woman is informed about the steps to take. Visit the link in the bio to delve deeper into what can be done. Together, let’s strive to put an end to the devastating impact of the disease and bring #DeathToCervicalCancer.”
Cervical Cancer: A Silent Killer
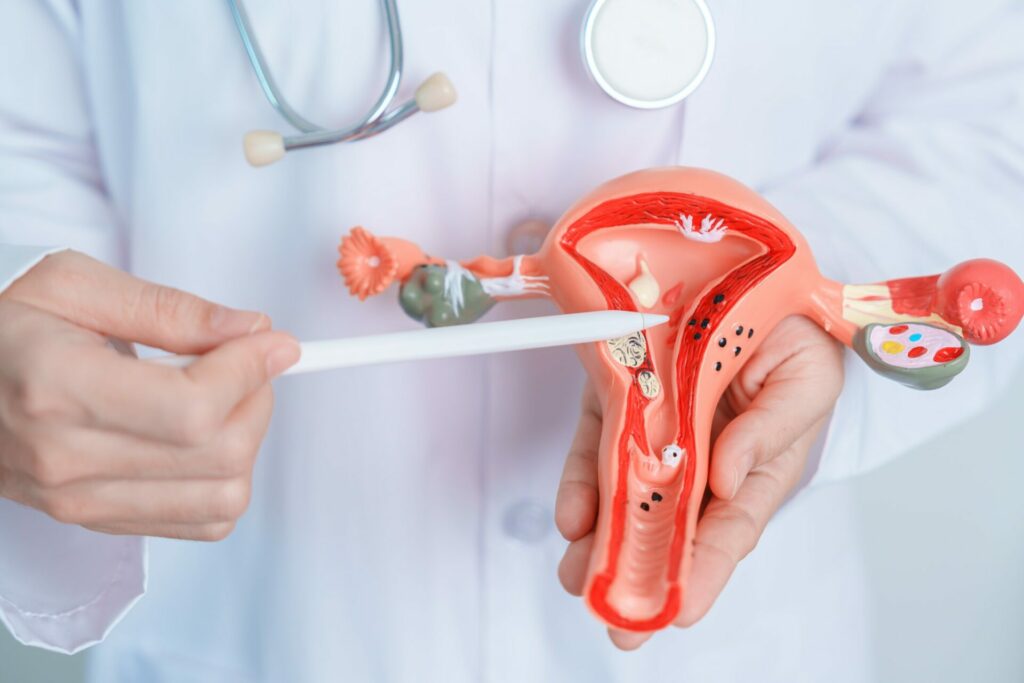
The cervix is a hollow tube that attaches the uterus to the top part of the vagina. Cervical cancer is a type of cancer that originates in the cells of the cervix. Cervical cancer develops when the cells of the cervix undergo abnormal changes due to the infection of human papillomavirus (HPV). HPV is a common sexually transmitted infection that can cause genital warts and cervical cancer.
Most people who are infected with HPV do not develop any symptoms or health problems, and the infection usually clears on its own. Although, in some cases, the infection persists and causes the cervical cells to grow and divide uncontrollably. This leads to the formation of precancerous lesions, which can progress to invasive cancer over time.
The development of cervical cancer is influenced by several factors, such as the type of HPV, the immune system, smoking, and other infections. The process of cervical cancer development can take years or even decades, and it can be detected and treated at an early stage through regular screening tests, such as Pap smears and HPV tests.
Cervical cancer can take as long as 15 to 20 years to develop in people with a healthy immune system. If you’re immunocompromised, i.e., have a weakened immune system, cervical cancer develops more quickly, at around five to 10 years.
What is HPV?
HPV (human papillomavirus) is the most common type of sexually transmitted infection (STI) in the United States and worldwide. HPV is passed between partners during vaginal, anal, and oral sex. It can also be transmitted through sex toys and intimate, skin-to-skin contact that doesn’t include penetrative sex.
In addition to cervical cancer, high-risk HPV strains can also cause other types of cancer. These include:
- Vaginal cancer
- Anal cancer
- Vulvar cancer
- Oropharyngeal cancer
- Penile cancer
High-risk HPV infection does not usually cause symptoms. That’s why cervical cancer screening is so important.
There are over 150 HPV virus strains. Most of these are low-risk. Some low-risk HPV strains may cause genital warts, but not cancerous changes to cells. Approximately 14 HPV viruses are high risk. These strains of HPV may cause cancerous changes within cells to occur. HPV16 and HPV18 are the ones most likely to cause cervical cancer.
Symptoms of Cervical Cancer

Cervical intraepithelial neoplasia is asymptomatic (no symptoms), so it’s important to see your healthcare provider for testing, even when you’re feeling fine. Any changes that worry you should also be checked out. The symptoms of cervical cancer can indicate other conditions as well. Symptoms include:
- Abnormal vaginal discharge
- Abnormal vaginal bleeding
- Low-back pain
- Pelvic pain
- Pain during vaginal sex
- Difficulty moving your bowels or urinating
- bleeding after a pelvic exam
- bleeding after you’ve gone through menopause
- abnormal vaginal bleeding, such as spotting between periods
- swelling of the legs
Stages of Cervical Cancer
If you have cervical cancer, the amount that it has spread will determine the stage of cancer you have. The International Federation of Gynecology and Obstetrics (FIGO) staging system is used to categorize cervical cancer spread.5 Cervical cancer stages range from 1 to 4. The lower the number, the less spread you have:
Stage 1: Cancerous cells have progressed from the surface of the cervix into deeper cervical tissues.
Stage 2: Cancerous cells have spread outside of the cervix and uterus but have not penetrated the pelvic walls or spread into the lower portion of the vagina.
Stage 3: Cancerous cells have spread into the lower vagina or walls of the pelvis. At this stage, a tumor may be blocking the ureters (tubes that carry urine from the kidneys to the bladder).
Stage 4: The cancer has metastasized (spread) into the bladder or rectum or distant areas of the body, such as the bones or lungs.
What are the risk factors of Cervical Cancer?
In addition to HPV, several risk factorsTrusted Source are known to have a link to cervical cancer. These include:
- contracting herpes or chlamydia
- smoking
- being exposed to the medication diethylstilbestrol (DES) in your mother’s womb
- having limited access to medical care and Pap testing
- having unprotected sex at a young age and with someone who’s considered high-risk for HPV
- having more than three full-term pregnancies or getting pregnant while very young
- those with limited access to screenings (Pap smears) or who choose not to screen
Your risk of HPV and other STIs goes up any time you have unprotected sex of any kind. Your risk for HPV also goes up if you started having unprotected sex at a young age and if you’ve had sex with someone who’s considered high-risk for HPV.
In addition, people who have a weakened immune system are at higher risk for acquiring an HPV infection, and thus cervical cancer. For example:
- those with HIV
- those with cancer
- transplant recipients
- those on immunosuppressive medications such as steroids
How can we prevent Cervical Cancer?
Strategies for cervical cancer prevention include proactive lifestyle choices, vaccination, and screening.
HPV vaccination is the best tool for preventing cervical cancer before it can start. Indian scientists have recently developed ‘Cervavac’, the first indigenous Human Papilloma Virus vaccine that can prevent cervical cancer and other HPV-associated cancers.
Poonam Pandey’s death hoax drew a major attention to cervical cancer, that stirred significant controversy. This public stunt for the awareness of cervical cancer and been a cause of death took a new turn when our Honourable Finance Minister, Nirmala Sitharaman, mentioned it during the Union Budget. “This act by Poonam has now resulted in making ‘Cervical Cancer’ and its related terms the most searched topic(s) on Google. This is the first time in the history of this country that the word ‘Cervical Cancer’ has been on thousand plus Headlines,” it read.
Sitharaman said that the government will encourage vaccination against HPV among girls in the age group of 9-14 years for the prevention of cervical cancer, the details about the programme were not revealed. According to an ANI report, the government is exploring options to cap prices so that the vaccines to treat cervical cancer become more affordable. The report suggests that, apart from slashing prices, the government will encourage HPV vaccination for cervical cancer through Information, Education and Communication (IEC) activities.
Takeaway – Cervical Cancer and Poonam Pandey
In India, cervical cancer is the second most common cancer and causes a quarter of the world’s cervical cancer deaths, even though it can mostly be prevented. Every year, around 1.25 lakh women in India are diagnosed with cervical cancer, and over 75 thousand die from it. In India, 83% of invasive cervical cancers are linked to HPVs 16 or 18, compared to 70% worldwide.
Cervical cancer develops slowly. It can take decades for an HPV infection to become cervical cancer. Fortunately, this means there’s plenty of time to detect any abnormal changes to your cervix that indicate cervical cancer. The early stages of cervical cancer are very treatable. You’ll likely have surgery to remove the cancerous tissue and any nearby areas to which it has spread.
This stunt by Poonam Pandey brought a whole new level of awareness about Cervical Cancer and how you can prevent it. It glorified the presence of a vaccine, a viable cure, rather than hiding and neglecting the disease. This ailment can be detected and prevented at an early stage if diagnosed properly.



